The therapeutic effects of high-dose melatonin administration
November 28th, 2016The therapeutic effects of high-dose melatonin administration
By Jesus A.F. Tresguerres1, M.D, Ph.D.
This article reviews the effects of high-dose melatonin administration on several diseases. Experimental studies performed over more than 20 years have shown that oxidative stress and inflammation increase in nearly all tissues with many degenerative diseases or aging. We have measured several parameters related to oxidative stress, inflammation and apoptosis both in several models of aging and also after ischemia in the liver or brain. The effect of treatment with melatonin has been evaluated showing a significant reduction of inflammation markers (tumor necrosis factor-alpha, interleukin 1 and 10, NFkBp50 and NFkBp52), apoptosis markers (BAD, BAX and Bcl2) and parameters related to oxidative stress, (heme oxygenases 1 and 2, endothelial and inducible nitric oxide synthases) in several tissues. Inflammations, as well as, oxidative stress and apoptosis markers were increased also in degenerative diseases like diabetes, hypertension or Parkinson disease so treatment with melatonin should also have very positive effects.
When the skin is submitted to ionizing radiation like radiotherapy a marked release of free radicals inducing inflammation and oxidative stress is obtained giving rise to radiodermitis. All of the above mentioned parameters have been also shown to be increased in the skin. Melatonin treatment was able to reduce those markers and oxidative stress preventing the appearance of radiodermitis.
The conclusion is that melatonin administration exerts beneficial effects against age- or degenerative diseases induced changes in several tissues and functions.
Introduction
According to the free radical theory of aging, which is one of the most widely accepted, the physiological decline that occurs with age is, at least in part, due to accumulative oxidative damage to cells and molecules. This oxidative damage is induced by reactive oxygen (ROS) and nitrogen (RNS) species, which are highly reactive. ROS have been implicated as major initiators of tissue damage and can up regulate enzyme activity, signal transcription, and gene expression of several compounds that can exert deleterious effects on proteins, lipids and DNA which in turn are responsible of all the age related alterations in the different tissues.
Cellular enzymatic antioxidant defenses which are present in young persons are able by scavenging ROS, to decrease the oxidative damage that could give rise to irreversible damages of structure and functions of cellular macromolecules. Loss of theses defenses with age enhances oxidative damage and has been suggested to contribute importantly to the aging process and to the pathogenesis of many age-related diseases.
Melatonin, an indolic hormone secreted by the pineal gland, is a substance closely related to biological rhythms and has been used since decades for the induction of sleep and the treatment of jet lag. In addition to its role as a chronobiotic hormone, melatonin is an ubiquitous direct free radical scavenger and an important indirect antioxidant. Moreover, melatonin is a small, lipophilic and hydrophilic molecule, what allows it to easily cross biological barriers and membranes, and diffuse throughout cell compartments, reaching the place where the free radicals and reactive species are generated in all tissues: the mitochondria.
Besides to these direct scavenging actions, melatonin stimulates also a host of endogenous antioxidant enzymes, including Superoxide Dismutase (SOD), glutathione peroxidase (GPx) and glutathione reductase (GRd), and inhibits the activity of Nitric oxide synthase (NOS) thus making possible to effectively fight against free radicals but also against inflammation, apoptosis and also in several age associated diseases.
In this paper a review of the effect of high doses of melatonin administration on several diseases related to oxidative injury are reviewed.
Melatonin and Diabetes type 2
Diabetes type 2 appears in the 4th decade of life in persons with a genetic predisposition and that generally show overweight. The first indication of glucose metabolism impairment is the appearance of peripheral insulin resistance. Pancreas reacts initially with beta cell hypertrophy leading to hyperinsulinemia and thus making it possible to maintain normoglycemia and later on, after some months or years, with beta cells getting exhausted or entering apoptosis with the corresponding reduction in plasma insulin levels and the appearance of hyperglycemia. Aging as well as insulin resistance has been shown to be associated with significant alterations in the expression of pancreatic genes involved in both insulin secretion and glucose metabolism.
Drugs used until now allow the treatment of diabetes as a chronic disease but are not able to cure it. The elements responsible for insulin resistance in peripheral tissues are related with oxidative stress and inflammation and the same occurs in the endocrine pancreas itself. Melatonin when given both to experimental animals (1-10 mg/Kg) that show already insulin resistance and hyperinsulinemia but also to humans (40-60 mg) with increased HOMA index, is able to revert the situation reducing plasma insulin levels and enhancing the islet production of insulin by reducing several inflammation and oxidative stress associated factors present both in the peripheral tissues like muscle or fat tissue such as TNF alpha, NFkB and IL1;2. The administration of melatonin to experimental animals was able also to increase in pancreas genes of survival like Sirt 1 and FOXO as well as genes of differentiation like PCNA, Pdx and Sei1 and to reduce apoptosis markers restoring its normal function.
These effects have been observed also in humans with insulin resistance in which besides of a reduction in plasma insulin levels a potentiation of the beta cell capacity to produce insulin, which reduces the risk of exhaustion of these cells and thus allowing the maintenance or restoration of normoglycemia.
Melatonin and skin – its topical effects
Some studies have been performed by our group to investigate also the role of melatonin in the aging skin showing an improvement in several parameters related to oxidative and inflammatory damage in the old skin. (Fig. 1)
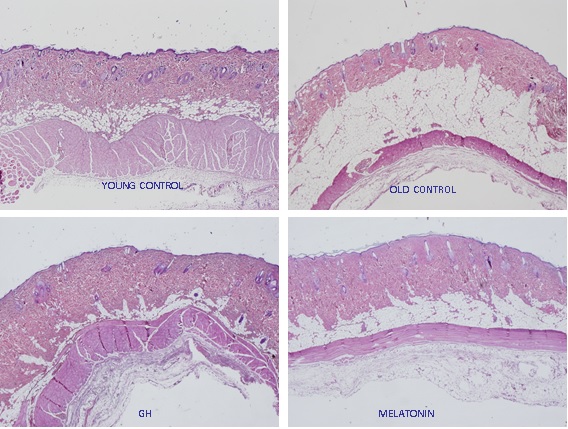
Figure 1: The effect of melatonin treatment for two months on the skin of old rats. When compared with the old control, an increase in epidermal thickness, a restructuration of dermis and a significant reduction of fat content of the hypodermis can be detected.
Radiotherapy is one of the most utilized treatments used in oncology to destroy tumoral cells. It is a local treatment in which only the area with sick cells is irradiated. Radiotherapy is used both as a principal, and as an adjuvant therapy together with other type of treatments such as surgery or chemotherapy, etc. The biological response to radiation starts with the generation of reactive oxygen species (ROS) This free radical excess released by ionizing radiations induces structural changes and damage in the cells that are sometimes irreversible.
The skin is the first barrier of defense of our organism from the outside and also is a rapid growing tissue. Thus, during radiotherapy, the skin, although not being the primary objective is at the end target of this therapy, since ionizing radiation needs to pass through it to arrive to the tumoral area. Hence, radiotherapy can produce adverse reactions, (radiodermitis) on the skin, during or after the treatment period.
In the majority of patients the effects of radiotherapy on the skin are scarce and transitory but in 20-25% of them, patients show severe reactions that are dependent of several factors that can predispose to radiodermitis: For example, total doses of radiation, doses per session, body area involved, genetic factors etc.
The application of a moisturizing cream with a 0.5% content of melatonin has been shown to very efficiently reduce the incidence of radiodermitis in women submitted to radiotherapy as complementary therapy after the surgical removal of mammary tumors. Normally after 15-20 sessions of radiotherapy the skin of the mammary gland is burned showing an important affectation. All the more than 30 women treated topically with melatonin showed no significant modifications of the skin.
Treatment of mucositis
When patients with several types of cancer are treated with chemotherapy and or radiotherapy, especially in the area of the throat or lungs very often all the mouth pharynx and gastrointestinal tract develops ulcers and inflammation on the mucosa, the so cold mucositis, which is associated with pain and great difficulties in eating. The administration of 1% melatonin in a specially developed gel that is first used for gargling and then swallowed 3 times a day completely prevents or cures the process. In our experience several patient have been treated with very good results. The method has been patented ad is in the final steps of approval by the European health authorities.
Treatment of Fibromyalgia
The pathogenesis of Fibromyalgia is at this time being unknown and the treatments assayed until now including corticoids, analgesics and opiates have shown no significant responses. However, the disease affects mainly women in their 4th or 5th life decades and is extremely debilitating. The possibility of the existence of a high level of oxidative stress and inflammation in this disease as indicated by high levels of C reactive protein, TNF alfa and IL1, opened the doors to a melatonin treatment that has shown very interesting results. In our experience, women are treated with doses ranging from 10 to 40 mg every day experience a very significant improvement in less than one month. The treatment needs to be maintained all the time taking also advantage of the sleep inducing properties of the compound. Women that were treated already with opiates could abandon these drugs and were able to reassume a normal life. My experience at this moment is of more than 20 women treated with a 90% rate of success.
Effect of Melatonin on ischemia reperfusion in the liver and brain
Ischemia/reperfusion injury of the liver or brain is a complex process involving numerous intracellular signalling pathways, mediators, cells, and pathophysiological disturbances The enhanced expression of these mediators’ leads to a second phase of injury characterized by the induction of secondary mediators that induce an additional damage.
The aging liver has been shown to display an increased susceptibility to Ischemia/Reperfusion (I/R), which may contribute to increased morbidity and postoperative mortality in liver transplantation which involves the maintenance of the donor liver in a protective solution at low temperatures. With increasing age, the capacity of liver cells against I/R damage is reduced due to decreased production of endogenous antioxidants and to a more evident inflammatory response, which might also contribute to the increased susceptibility for tumour growth. Other of the important age-related changes is a decrease in its regenerative capacity. Nevertheless, livers from older subjects have been used successfully for transplantation, although data published on 91 seniors who underwent transplantation at the University of Wisconsin showed poor long-term patient survival after receiving livers from older donors.
In our experimental approach, the expression of pro-inflammatory cytokines was significantly increased in liver after ischemia and 36 h of reperfusion. Our findings were in accordance with previous studies, in which an increase in pro-inflammatory cytokines, such as TNF-α, IL-6, IL1β was observed. In our research, the increased mRNA expressions of IL1β, MCP-1 and INFγ were more evident in older animals after I/R as compared with younger ones.
Treatment with melatonin significantly attenuated the increased level of serum aminotransferase, reduced the severity of hepatic cell damage, diminished steatosis and the immigration of inflammatory cells. Furthermore, melatonin was shown to decrease serum levels and tissue content of inflammatory cytokines (TNFα, IL6, IL1β, and MCP-1), to reduce neutrophil infiltration and to inhibit apoptosis of hepatocytes. Melatonin was able to ameliorate oxidative stress and to inhibit pro-inflammatory cytokines production and reactive oxygen species, protecting against hepatic damage.
The key mechanism of liver damage after I/R has been identified as increased apoptosis. Our results have shown also that melatonin treatment was able to diminish the expression of pro-apoptotic genes like Bax, AIF or Bad, together with restoring ATP content. So melatonin administered to donor livers probably could ameliorate the long term survival of patients by reducing the oxidative stress and inflammation and apoptosis induced by ischemia.
Another study from our group has initially developed a valid model for studying cerebral ischemic lesions induced by introducing a nylon catheter in the medial cerebral artery of rats. The achieved ischemia is associated with a very high release of free radicals shows a high damaging potential that is age dependent, being more important in the older animals.
Ischemic damage after the blockade of the medial cerebral artery determines a lesion that can be detected in the hippocampus and the cerebral cortex, with increases in TNF alpha or IL1 as markers of inflammation and with reduction of Bcl2 and the increase of BAX that are showing the increase of apoptosis.
The effect of treatment with melatonin (10 mg/ Kg/ bodyweight/ day) was investigated. A significant reduction in the inflammatory and apoptotic parameters was seen indicating a reduction in the size and intensity of the lesion. This opens the possibility of treatment of stroke with around 100 mg of melatonin.
Melatonin on the heart
In old experimental animals we have observed in the heart increased levels on mRNA expression of cytokines such as TNFα, IL-1β (Fig 6), HO-1, iNOS and NFkB together with a decrease in the expression of eNOS and IL-10.
Studies have also reported that oxidative stress can induce apoptosis in cardiac myocytes and that excessive ROS production can cause mitochondrial damage and dysfunction. All these situations lead to endothelial cell dysfunction in many diseases, such as hypertension with reduced availability of endothelial nitric oxide.
The existence of age-dependent increases in oxidative stress, in heart mitochondria of senescence prone mice has also been observed. Iinflammatory stimuli can induce the expression of iNOS in cardiocytes whereas endothelial NO synthase that is needed for a normal endothelial function is reduced.
Melatonin treatment for one month to 10 month old senescence prone mice exhibited improvements in inflammation and oxidative stress in the heart and was able to counteract the age dependent increased production of pro-inflammatory cytokines, (TNFα, IFNγ) and NO. It has been widely documented that, melatonin exerts its protective effect as a result of its antioxidant scavenging properties, its direct detoxification of free radicals and its ability to preserve efficient oxygen metabolism in mitochondria. These facts support the concept that melatonin exerts profound protective effects against aging, at least, blocking the inflammatory and oxidative processes.
Melatonin can also be used for the prevention of damage induced by ischemia in the heart. (Fig. 2) When given previously in a similar way than in the liver or brain the substance is able to reduce the areas of necrosis after coronary obstruction.
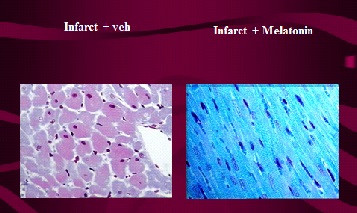
Figure 2: The effect of melatonin treatment on experimental myocardial infarction.
Melatonin and Parkinson disease
Parkinson disease appears when the dopamine producing neurons of the basal ganglia from and specially the substantia nigra degenerate, depleting the striatum from dopamine. When the number of surviving dopaminergic neurons arrives at less than 20% of the original number, the disease appears with a combination difficulty to initiate movements, the muscles becoming rigid and showing a characteristic resting tremor. Untreated these signs gradually worsen rendering the patients at the end totally unable to move voluntarily.
Restoring the dopamine content of the brain by giving the precursor L-dopa that crosses the blood brain barrier is able to significantly ameliorate the disorder by increasing the amount of dopamine in the substantia nigra allowing the increase in the amount of dopamine available at the synapses of the striatum. L-dopa treatment however does not cure Parkinson disease and in fact the continuous degeneration of the dopaminergic neurons leads to a reduction in the treatments effectivity. Also although the transplant in the substantia nigra area of dopaminergic neurons obtained from different sources like the carotid body or the adrenal medulla is able to significantly ameliorate the disease, with time ,also the transplanted neurons undergo degeneration and the effect can be abolished.
Degeneration of the dopaminergic neurons is caused finally by increased oxidative stress and inflammation. Treatment with melatonin at doses between 25 mg and 100 mg are able to significantly reduce oxidative stress in the substantia nigra thus blocking neuron death. This treatment needs to be started at the initial steps of the disease since it is not able to reverse the already degenerated neurons. The combined treatment with L-dopa and melatonin reduces the doses needed of the dopamine agonist and blocks the evolution of the disease, by preventing the oxidative stress induced neurone death. The disease remains stable and does not continue its evolution.
Alzheimer disease and melatonin
Alzheimer disease is responsible of nearly 70% of cases of dementia. The reason behind involves the degeneration of cortical neurons thin cortical gyri and enlarged ventricles is the hallmark of the disease as observed by NMR. The pathogenesis of the disease involves the presence of Amyloid plaques in the gray matter of neocortex and hippocampus of the brain although it is not clear how the deposition of this protein leads to the degeneration of neurons or ever if this substance is the real causative agent of the disease or is only an inert byproduct of neuronal death. Neurofibrillary tangles are bundles of abnormal filaments inside the pyramidal neurons as well as neuronal cell loss and changes in cellular morphology are also present in the disease.
The storage of new memory is affected very early but at the end also the previously stored memory become impaired. Patients eventually lose interest at there surroundings and become confined to wheelchair or bed. The disease can last 5 to 10 years until the total loss of body functions.
The central question is why neurons die in Alzheimer disease. Although several theories have been proposed, including the reduction of several growth factors it is becoming clear that again excitotoxicity leading to oxidative stress is at the end the most likely pathogenic pathway. Taking this into consideration, treatment with melatonin has been considered. The first study was undertaken in Argentina where two identical male twins developed Alzheimer at the same time. Since one was living in Buenos Aires, one had the opportunity of being treated with melatonin whereas the other was not treated. Five years later the non-treated patient died whereas the melatonin treated remained in a mild form of disease. From this moment on, other clinical trials have been carried out in which melatonin treatment was first able to allow a normal sleep patterns in those patients without the sun-downing effect. In addition and specially those patients with a very initial form of the disease showed a slowing down in the evolution of the disease. The doses used have been between 3 mg and 25 mg per day. No secondary effects were observed. Also no side effects were recorded by using 100 mg at bedtime for several years.
Malignant epilepsy
Some patients suffer a very severe form of epilepsy that includes high intensity seizures 3 to 6 times a day. In children this is associated with high level of brain damage leading to death in several months. One case of a 3 year old girl was treated with 100 mg of melatonin at bedtime plus 10 mg in the morning for some months obtaining a nearly complete normalization of the electrical activity of the brain and a dramatic amelioration of the clinical situation. (Fig. 3) If the treatment was removed, the original situation appeared again.
Figure 3: The basal EEG registration of a 3 year old girl with malignant epilepsy. Registration after 2 months of treatment with 100 mg melatonin shows a completely normal electrical activity under treatment.
References
- Department of Physiology, School of Medicine, Complutense University, Madrid, Spain.
- Albarran, MT, S Lopez-Burillo, M I Pablos, R J Reiter, M T Agapito, 2001, Endogenous rhythms of melatonin, total antioxidant status and superoxide dismutase activity in several tissues of chick and their inhibition by light: J Pineal Res, v. 30, p. 227-233.
- Azcoitia, I., Pérez-Martín, M., Salazar, V., Castillo, C., Ariznavarreta, C.,Garcia-Segura,LM and Tresguerres, J.A.F. “Growth hormone prevents neuronal loss in the aged rat hippocampus”. Neurobiology of Aging 26: 697-703, 2005
- Benot,S, R Goberna, R J Reiter, S Garcia-Maurino, C Osuna, J M Guerrero, 1999, Physiological levels of melatonin contribute to the antioxidant capacity of human serum: J.Pineal Res., v. 27, p. 59-64.
- Cagnoli, CM, C Atabay, E Kharlamova, H Manev, 1995, Melatonin protects neurons from singlet oxygen-induced apoptosis: J Pineal Res, v. 18, p. 222-226.
- Cardinali DP1, Furio AM, Brusco LI. The use of chronobiotics in the resynchronization of the sleep/wake cycle. Therapeutical application in the early phases of Alzheimer’s disease. Recent Pat Endocr Metab Immune Drug Discov. 2011 May;5(2):80-90.
- Castillo C, Salazar V, Ariznavarreta C, et al. Effect of melatonin administration on parameters related to oxidative damage in hepatocytes isolated from old Wistar rats. J. Pineal Res 2005; 38:240-246
- Cheung,RT, 2003, The utility of melatonin in reducing cerebral damage resulting from ischemia and reperfusion: J.Pineal Res., v. 34, p. 153-160.
- FitzGerald, Bishop M, Tillman G, Aronowitz J, Pieters R, Balducci S et al. Radiation therapy toxicity to the skin. Dermatol Clin 2008;26: 161-72
- Fisher TW, Slominski A, Zmijewski MA, Reiter RJ, Paus R. Melatonin as a major skin protectant: from free radical scaveniging to DNA damage repair. Exp Dermatol 2008; 17:713-30
- Fischer TW, Zmijewski MA, Worstman J, Slominski A. Melatonin mantains mitocondrial membrane potential and attenuates activation of initiator (caspasa 9) and effector caspases (casp-3/casp-7) and PARP in UVR-exposed HaCaT keratinocytes. J Pineal Res 2008; 44:397-407
- Fischer TW, ELsner P. Melatonin: a hormone, drug or cosmeceutical. In: Elsner P, Maibach H leds. Cosmeceuticals and Active Cosmetics, Vol 1. Boca Raton: Taylor&Fancis, 2005:413-19
- Fischer TW, Greif C, Fluhr JW, Wigger-Alberti W, Elsner P. Percutáneous penetration of topically applied melatonin in a cream and an alcoholic solution. Skin Pharmacol Physiol 2004;17:190-94
- Hymes S, Strom E, Fife C. Radiation dermatitis: clinical presentation, pathophysiology, and treatment. J Am Acad Dermatol 2006; 54:28-46
- Ianas,O, R Olinescu, I Badescu, 1991, Melatonin involvement in oxidative processes: Endocrinologie, v. 29, p. 147-153.
- Kireev RA, Tresguerres ACF, Castillo C, Salazar V, Ariznavarreta C, Vara E, and Tresguerres JAF
- “Effect of exogenous administration of melatonin and GH on prooxidant functions of the liver in aging male rats
- Pineal Research 42;64-70 (2007)
- Ling,X, L M Zhang, S D Lu, X J Li, F Y Sun, 1999, Protective effect of melatonin on injuried cerebral neurons is associated with bcl-2 protein over-expression: Zhongguo Yao Li Xue.Bao., v. 20, p. 409-414.
- Magri,F, S Sarra, W Cinchetti, V Guazzoni, M Fioravanti, L Cravello, E Ferrari, 2004, Qualitative and quantitative changes of melatonin levels in physiological and pathological aging and in centenarians: J.Pineal Res., v. 36, p. 256-261.
- Manev,H, T Uz, A Kharlamov, J Y Joo, 1996, Increased brain damage after stroke or excitotoxic seizures in melatonin-deficient rats: Faseb Journal, v. 10, p. 1546-1551.
- Matsubara E, Bryant-Thomas T, Pacheco Quinto J, Henry TL, Poeggeler B, Herbert D, Cruz-Sanchez F, Chyan YJ, Smith MA, Perry G, Shoji M, Abe K, Leone A, Grundke-Ikbal I, Wilson GL, Ghiso J, Williams C, Refolo LM, Pappolla MA, Chain DG, Neria E. Melatonin increases survival and inhibits oxidative and amyloid pathology in a transgenic model of Alzheimer’s disease. Neurochem. 2003; 85:1101-1108.
- Melchiorri,D, R J Reiter, E Sewerynek, L D Chen, G Nistico, 1995, Melatonin reduces kainate-induced lipid peroxidation in homogenates of different brain regions: FASEB J, v. 9, p. 1205-1210.
- Mordenti Jy Chappel W The use of interespecies scaling in toxicokinetics en (Yacobi ,Kelly y Batra V)eds Toxicokinetics and new drug development
- Pergamon press New York 1989 pp42-96
- Reiter,RJ, 1998, Oxidative damage in the central nervous system: protection by melatonin: Prog.Neurobiol., v. 56, p. 359-384.
- Reiter,RJ, 2003, Melatonin: clinical relevance: Best.Pract.Res.Clin.Endocrinol.Metab, v. 17, p. 273-285.
- Reiter,RJ, D X Tan, S Burkhardt, 2002, Reactive oxygen and nitrogen species and cellular and organismal decline: amelioration with melatonin: Mech.Ageing Dev., v. 123, p. 1007-1019.
- Sastre,J, F V Pallardo, J Vina, 2000, Mitochondrial oxidative stress plays a key role in aging and apoptosis: IUBMB.Life, v. 49, p. 427-435.
- Shirazi A, Ghobadi G and Ghazi-Khansari M. A radiobiological Review on Melatonin: a novel radioprotector. J. Radiat. Res. 2007; 48:2063-72
- Tan,D, L Chen, B Poeggeler, L Manchester, R Reiter, 1993, Melatonin: a potent, endogenous hydroxyl radical scavenger: Endocr.J, v. 1, p. 60-87.
- Tan DX, Manchester LC, Terron MP, Flores LJ, Reiter RJ. One molecule, many derivatives: a never-ending interaction of melatonin with reactive oxygen and nitrogen species. J Pineal Res 2007; 42:28-42
- Tresguerres JAF, Kireev R, Tresguerres ACF, Borras C Vara E , y Ariznavarreta C Mecanismos moleculares del envejecimiento y su prevencion mediante tratamiento hormonal en ratas.
- Tricoire,H, A Locatelli, P Chemineau, B Malpaux, 2002, Melatonin enters the cerebrospinal fluid through the pineal recess: Endocrinology, v. 143, p. 84-90.
- Witt-Enderby PA, Bennett J, Jarzynka MJ, Firestine S, Melan MA. Melatonin receptors and their regulation: biochemical and structural mechanisms. Life Sci. 2003; 72: 2183-2198.
- Wakatsuki, A. Y Okatani, K Shinohara, N Ikenoue, C Kaneda, T Fukaya, 2001, Melatonin protects fetal rat brain against oxidative mitochondrial damage: J Pineal Res, v. 30, p. 22-28.