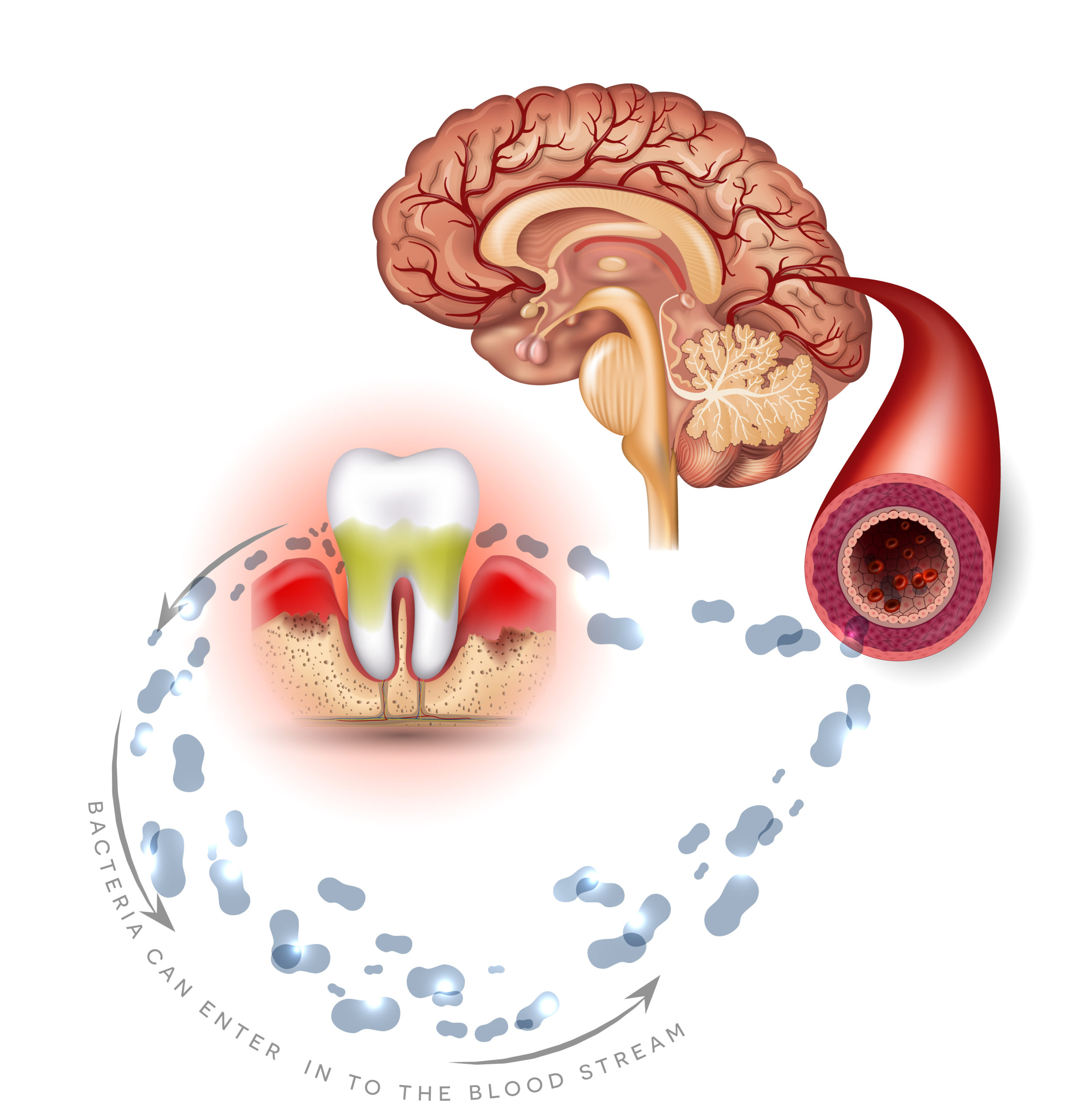
Wash your mouth out!
November 23rd, 20178 things that you should know about your mouth
Bacteria growth
A once and for all cure to get rid of bad bacteria doesn’t exist, they will always be present and your priority should be to protect your mouth from invasion!
The bacteria streptococci and staphylococci are commonly known and present in most serious diseases and conditions. Just because you don’t see the bacteria, doesn’t mean to say you don’t have them. Having bacteria in your mouth is normal but do not ignore their existence. The consequences could be devastating. Managing the bacteria community in your mouth can be done by daily brushing, flossing your teeth and using a mouth wash. Sometimes even this is not enough, so regular visits to the dentist is very important.
It isn’t just your teeth and gums that you should be concerned about when it comes to bacteria. Complications from bacteria in your mouth could be connected to life threatening diseases. Always seek advice if you have concerns. It’s not just brushing your teeth and using a mouth wash that is important, it’s what you put in your mouth too. Bad management of oral bacteria can lead to oral infections and viruses. The Dental Clinics of North America produced a very insightful article about oral viral infections caused by bacteria. It details the commonly seen viral infections in the oral cavity with associated systemic manifestations. It encompasses viral infections discussing clinical features, histopathology, diagnosis, treatment and prevention. (1)
Oral infections
There are many types of bacteria related oral infections:
- Dental caries or cavities caused by a build-up of bacteria are the leading cause of tooth loss
- Gingivitis is when bacteria settle in the gum’s crevices and the bacteria turn into toxins. The gums react by becoming inflamed and swollen
- Gingivitis that spreads below the gum line and effects the bones and tissues can result in periodontal disease. The teeth can loosen and is another common cause of tooth loss in adults
- Hand, Foot and Mouth Disease is most likely to develop in children and the virus Coxsackie A16 is usually responsible. Symptoms start with a fever, slightly painful blisters can appear inside the cheeks and the tongue
- Herpangina is related to hand, foot and mouth disease. Most frequently infects children aged 3-10. Symptoms start with a sore throat and difficulty swallowing. Tiny blisters develop at the back of the mouth which form large ulcers and eventually they rupture
- Thrush is an overgrowth of the naturally occurring bacteria ‘Candida albicans’. It requires medical treatments such as antibiotics. Symptoms are a white curd-like plaque which can appear on the tongue, inner cheeks, palate and back of the mouth
- Canker sores are lesions that start on the gums and other mouth tissues. Medically known and apthous ulcers
- Oral Herpes is caused by the herpes simplex virus. Symptoms can be much like flu, blisters and ulcers may be present on the tongue
The American Society of Clinical Oncology (ASCO) produced one of the first large studies to explore the possible impact of HPV vaccination on oral HPV infections; researchers found it may confer a high degree of protection. The study of young adults in the United States showed that the prevalence of high-risk HPV infection was 88% lower among those who reported getting at least one vaccine dose than among those who were not vaccinated. (2)
Gum disease
Gum disease is otherwise known as Gingivitis or Periodontal disease and it is a common dental problem. Nearly 3 out of 4 people over the age of 35 have it to some degree. It is the common reason for tooth loss in adults. It can be identified by swelling, inflammation or infection of the gums and other tissue that holds your teeth in place.
Gingivitis is inflamed gum tissue around the teeth, caused by dental plaque which is responsible for cavities. Healthy gums are generally coral-pink in color and firmly attached to the teeth. The first sign of gingivitis is bleeding gums during brushing and the gums may be tender to touch. This is a reversible condition that can be improved by good dental hygiene. Periodontal disease is a more severe form of the condition. This is where the bone and other foundations that hold the teeth in place are stripping away.
The University of Louisville School of Dentistry researchers have found a bacterial species responsible for gum disease, Porphyromonas gingivalis, is present in 61 percent of patients with esophageal squamous cell carcinoma (ESCC). The findings, published recently in Infectious Agents and Cancer, only detected P. gingivalis in 12 percent of tissues adjacent to the cancerous cells, while this organism was undetected in normal esophageal tissue.
“These findings provide the first direct evidence that P. gingivalis infection could be a novel risk factor for ESCC, and may also serve as a prognostic biomarker for this type of cancer,” said Huizhi Wang, M.D., Ph.D., assistant professor of oral immunology and infectious diseases at the UofL School of Dentistry. “These data, if confirmed, indicate that eradication of a common oral pathogen may contribute to a reduction in the significant number of people suffering with ESCC.”
This is the first study to evaluate the association of bFGF and TGF-b on human periodontal ligament cells. Based on previous reports, two concentrations of these growth factors were used in order to assess a possible dose-response effect. A dose-dependent effect on cell proliferation was expected for bFGF, whereas a time-dependent effect was anticipated for TGF-b stimulation. Surprisingly, neither of the concentrations of bFGF stimulated cell proliferation. Since bFGF had other biological effects on these cells we assume the hPDL fibroblasts express the adequate receptors.
Things that will increase the risk of gum disease are:
- Smoking – this greatly increase the risk of developing problems and also increases the severity and rate of the tissue destruction
- Poorly controlled diabetes
- Pregnancy
- Certain medications
- Age – problems increase as you age
Bad breath
Halitosis is otherwise known as bad breath. It is when a bad odour comes from the mouth. There are a variety of causes, eating certain foods or bad dental hygiene. Halitosis is normally caused by bacteria. Bacteria builds up, forming plaque on the teeth, on the gums and also on the tongue. Bacteria grow well in a warm and wet oral environment, when levels are high, smelly odours are released.
Our breath odour varies throughout the day, after drinks or food or morning breath.
These are some of the factors that can cause bad breath:
- Bad oral hygiene
- Gaps between the teeth that fill up with plaque
- Gum disease
- Smoking
- Strong flavoured foods such as garlic or onions
- Coffee
- Alcohol
- Medications that cause dry mouth
- Infections in the respiratory tract such as infections in the lungs or throat
- Illnesses from other parts of the body, kidney failure, diabetes, liver disease or lung disease
- Eating disorders
A study was conducted by Francisco Wilker Mustafa Gomes Muniz, Stephanie Anagnostopoulos Friedrich, Carina Folgearini Silveira and Cassiano Kuchenbecker Rösing for the Journal of Breath Research. They aimed to analyze the impact of chewing gum on halitosis parameters. Three databases were searched with the following focused question: ‘Can chewing gum additionally reduce halitosis parameters, such as organoleptic scores and volatile sulfur compounds (VSC), when compared to a control treatment’? Chewing gum containing sucrose was able to reduce the VSC levels, in comparison to xylitol and zinc citrate chewing gum, but only for 5 min. It was concluded that chewing gums containing probiotics Lactobaccilus, zinc acetate and magnolia bark extract, eucalyptus-extract, and AITC with zinc lactate may be suitable for halitosis management. (4)
Your mouth and tongue
Whatever mouth and tongue discomfort you experience whether it’s from dental problems or mouth ulcers it is important that you deal with it straight away. A build-up of bacteria can cause abscesses or be an indication of something even more serious. One condition that is a cause for concern is burning mouth syndrome. The symptoms may last for months or years! Or in some cases symptoms may suddenly disappear on their own, or become less frequent. Some sensations can be alleviated during eating or drinking. The condition doesn’t normally show physical changes to your tongue or mouth.
Symptoms of burning mouth syndrome:
- A sensation of a dry mouth with increased thirst
- A burning or scalded sensation that has an effect the tongue the lips, gums, palate, throat or whole mouth. It depends on the severity
- Taste changes such as a metallic or bitter taste
- A loss of taste altogether
Causes of burning mouth syndrome:
- When no clinical abnormalities are identified the condition is called idiopathic burning mouth syndrome. In this instance the condition could just be nerve related
- Sometimes the condition can develop from an underlying medical condition
- Various medications
- Fungal infection – oral thrush or lichen planus
- Nutritional deficiencies
- Dentures
- Allergies or reactions
- Reflux
- Oral bad habits
- Endocrine disorders
- Excessive tooth brushing or abrasive toothpastes
- Anxiety, depression or stress
- Abrasive toothpastes, overusing mouthwashes or having too many acidic drinks
The main symptom of burning mouth syndrome (BMS) is pain in the mouth that is burning, scalding, or tingling. Or, the pain may be a feeling of numbness. Other symptoms include dry mouth or altered taste in the mouth.
BMS is a painful condition. Usually, the tongue is affected, but the pain may also be in the lips or roof of the mouth, or throughout the mouth.
BMS pain can last for months or years. Some people feel constant pain every day. For others, pain increases throughout the day. For many people, the pain is reduced when eating or drinking. The National Institute of Dental and Craniofacial Research explain that the diagnosis of BMS is difficult to do. Multiple tests would have to be done – blood, oral swab, allergy and salivary flow tests. (5)
Damaged enamel and cavities
Tooth decay is also known as dental caries or cavities. It is the destruction of teeth caused by plaque acids. There are three main causes of tooth decay, bad bacteria, food and drinks. Bacteria are found in dental plaque, plaque is the thin white film that is constantly forming on your teeth after you brush. The bacteria produces harmful acid which erodes the tooth, this can lead to cavities. Sugars and carbohydrates in food are the main dangers to the teeth, bacteria and plaque loves them! They feed on the sugars and carbohydrates and turn them into plaque acids. This attack can last for at least an hour until saliva helps to neutralize the acid. The frequency of taking on those types of foods and drinks is more harmful than the amount.
Typical foods and liquids would be: Candy, chocolate, fizzy drinks, juice, biscuits, ice cream, jam, jelly, fruits, potato chips, cereals, pretzels and yoghurts. There are a lot of hidden sugars in foods too.
Decay is a gradual process. Decay occurs in different areas of the tooth. Grooves, pits or fissures, the surface between teeth, near the gum line, around fillings, crowns, partial dentures and bridgework
Acid erodes the tooth enamel, a small white spot may be seen and at this point it is still possible to reverse the damage. But, if left untreated, the damage with continue through to the softer part of the tooth called dentine, this is when the cavity is form. The decay will eventually reach the dental pulp where the nerves are and potentially a root canal or tooth extraction could be required.
Tooth decay symptoms:
- Sensitivity to cold or hot food or drinks
- Toothache
- Bad breath
- Throbbing in the mouth
- Discomfort when eating
Tooth decay is a common disorder, second only to the common cold. It usually occurs in children and young adults, but it can affect anyone. (6)
Enamel remineralization
Our saliva has healing properties. Naturally occurring proteins, enzymes and cellular compounds in saliva can fight some infections and slow down tissue loss as infection penetrate open or broken layers of skin. Those compounds help our teeth, they work to harden or ‘remineralize’ the enamel on the teeth.
Teeth are strong on the exterior because of tight mineral bonds of enamel. It’s one of the strongest substances in the human body. Saliva is watery but has properties strong enough to help keep the teeth strong. It keeps calcium and phosphates flowing around the mouth so teeth can remineralize. If it wasn’t for saliva and its healing properties, teeth would lose their hard-coated enamel covering; bad bacteria and acids would penetrate the enamel to the dentin. Teeth would become soft and chewing would be difficult.
Soft teeth would be no match for food that needs to be broken down before getting digested in the stomach and the very nutrients needed to keep the body and the teeth healthy would be hard to absorb.
In a regular or normal mouth, teeth will stay tough and protected but sometimes bacteria and acids win the battle and overtake the saliva balance, leading to plaque, tooth decay and cavities. Poor hygiene, a high-sugar or acidic diet, and tooth damage increase demineralization, as can illness and medication, so knowing how remineralization works can help you keep your enamel and teeth strong.
A recent study from Scientific Reports – In vivo remineralization of dentin using an agarose hydrogel biomimetic mineralization system reported the use of an agarose hydrogel biomimetic mineralization system loaded with calcium and phosphate to induce dentin remineralization and formation of a oriented densely parallel packed HA layer on dentin surface in a rabbit model in vivo. The results indicated a potential clinical use for repairing dentin-related diseases, such as erosion, wear, and dentin hypersensitivity. (7)
Shrinking gums
Shrinking gums or ‘receding gums’ refer to exposure of the roots of your teeth. Roots are normally coated in healthy tissue called gingiva. Shrinking gums are a common problem in adults who are over 40, although, in some cases it can start in teenage years. Symptoms develop over time, teeth appear longer, teeth and gums become sensitive and a bump or series of bumps can be felt along your gum line. If the gingival tissue appears swollen, it could result in bleeding gums or bad breath. The gaps between crowns or bridges may become wider too and the dark line of the crown will be revealed.
The cause:
- Poor oral hygiene, smoking, medical conditions, trauma to the gums
- Over-aggressive brushing – this action can wear down enamel
- Crowding – this can lead to one or more teeth lying out of line of the arch
- Grinding – the action of grinding or clenching is another possible cause
- Anug – a nasty infection that it more common in younger people
- Periodontal disease – a progression from gingivitis
- Genetic predisposition – some people have thin or insufficient gingival tissue and some develop high frenum. These are little tags that connect your gums to the cheeks/lips
- Dental treatments – ill-fitting crowns or dentures
There are easy steps that you can take to reduce the risk of oral bacterial infections. Good oral hygiene, flossing, mouthwash, dental check-ups and dental scaling. Seek advice about correct brushing techniques and using an appropriate toothbrush that suits your mouth and gums. Ill-fitting dental work should be fixed and sensitive teeth should be dealt with. With more serious conditions there are further treatments that you can have:
- Saliva replacement products
- Specific oral rinses or lidocaine
- Capsaicin, a pain reliever that comes from chili peppers
- An anticonvulsant medication called clonazepam (Klonopin)
- Certain antidepressants
- Medications that block nerve pain
- Cognitive behavioural therapy
It is reported that one hundred and fourteen million Americans don’t have insurance coverage for their teeth!
The American debate on oral health
According to an article in the New York Times, Americans are debating medical coverage and the problem of their teeth has remained almost entirely unaddressed. About 114 million Americans don’t have insurance coverage for their teeth. That is more than the number of people who didn’t have health insurance before the Affordable Care Act.
“Oral health is a neglected issue nationally,” said Julia Paradise, an associate director of the program on Medicaid and the Uninsured at the Kaiser Family Foundation. “This is a big problem. The mouth and the head – mental health and dental health – somehow remain outside of what people think of as general health.” (8)
A healthy mouth is about good dental hygiene, regular dental check-ups and a healthy diet.
Wash your mouth out because prevention is better than cure!
OralTide-Pro is a mouthwash containing DPR (Dental Bond Peptide) and AGDP (Anti-gingival Degenerate Peptide).
Dental Bond Peptide is refined and obtained from mass production of enriched fermented peptides using patented hydrolysis technology to yield a high concentration of precise DRP fragments and then purified via ultrafiltration membrane technology.
Anti-gingival peptide is refined and obtained from mass production of enriched fermented peptides using patented hydrolysis technology to yield high concentration of precise AGDP fragments and then purified via ultrafiltration membrane technology. AGDP can increase synthesis of type 1 collagen and extracellular matrix repairs the fracture and breakage of collagen organization. It promotes growth of shrinking gums, accelerates mouth tongue wound healing, and relieves symptoms of inflammation of the gums by activating gingival connective tissue and periodontal ligament fibroblasts.
The 4 guarantees of OralTide-Pro:
- No bactericide and no alcohol.
Bactericide may be carcinogenic (a substance that promotes formation of cancer) and excessive alcohol can thin the oral mucosa which may lead to being carcinogenic.
- No fluoride.
Excessive fluoride may cause fluorosis on the teeth (a mottled effect), nerve injury of the brain, spinal cord or sciatic nerve.
- No potassium nitrate.
Potassium nitrate has a narcotic effect which will reduce the sensitivity of the tooth nerve potentially leaving tooth decay unnoticed.
- Qualified by SGS.
Comparison table of OralTide-Pro and a commercial dental care product:
| Item | Active ingredients | Function | Commerical mouthwash | OralTide-Pro |
| Fluorides | Sodium fluoride, sodium monofluorophosphate | Anti-caries | Added | No additives |
| Supplementary enamel | Zinc hydroxyapetite | Enamel remineralization | No additives or added | DPR-Ca |
| Bactericide | Gluconic acid chlorhexide, cetyl pyridinium chloride | Anti-caries | Added | Xylitol |
| Anti-inflammation | Allantonin, licorice acids and salts | Prevent gum inflammation | No additives or added | AGDP |
| Anti-sensitive | Potassium nitrate, strontium chloride | Anti-hypersensitivity | Added 1-5% potassium nitrate | No additives |
| Alcohol | Ethanol | Sterilize | No additives or added | No additives |
| Treatment of gingival recession | AGDP | Repair gingival recession, oral and gingival anti-inflammation, repair oral popi and wound | No additives | AGDP |
| Treatment of enamel remineralization | DRP – Ca complex | Damaged enamel remineralization, anti- hypersensitivity | No additives | DRP-Ca |
FAQ
What are AGDP/DRP sources?
Edible AGDP/DRP are refined and obtained from mass production of enriched fermented peptides using patented hydrolysis technology to yield a high concentration of precise peptide, and then purified via ultrafiltration membrane technology.
Have AGDP/DRP got any side effects?
Peptides in the body within 4-8 hours will be metabolized into amino acids and it does not build up in your organs. Compared with other drugs, peptides are less likely to cause side effects.
What is the role of peptides in dental care therapy?
A peptide is a protein fragment consisting of two or more amino acids. Specific sequence AGDP/DRP can act directly on the affected area and have high efficacy and specificity in the mouth.
What is the role of peptides in the enamel?
DRP can transport and deposit calcium ion into the damaged enamel microstructure to remineralize, fill the slot, reduces bacterial growth and prevents etching.
What is the role of peptides in the gum?
Promoting collagen and extracellular matrix (ECM) synthesis, activating growth factors to accelerate mouth healing such as tongue wounds. Healing, promoting growth of shrinking gums and relieving symptoms of inflammation of the gums.
How long will the product be effective?
Anti-sensitive teeth: 1 week of continued use. Wound healing/anti-inflammation: 6 times of continual use. Growth of shrinking gums: 2 months of continual use.
How to use OralTide-Pro
1ml OralTide-Pro mixed with 10ml water. Hold in mouth for 5-10 minutes 1-2 times a day.
Open wide for OralTide-Pro and feel confident about your mouth.
References:
- Oral infections: Diagnosis and Management. Dental Clinics of North America.
Volume 61, Issue 2 – April 2017, pages 351-363. Earl Clarkson, DDS, Saif Abulateef, DDS,
Fatima Mashkoor, DDS. https://doi.org/10.1016/j.cden.2016.12.005
- American Society of Clinical Oncology (ASCO). “HPV vaccination may reduce oral HPV infections, but still under-utilized.” ScienceDaily. ScienceDaily, 18 May 2017. Wikesjo UM, Nilveus RE, Selvig KA.
- Shegan Gao, Shuoguo Li, Zhikun Ma, Shuo Liang, Tanyou Shan, Mengxi Zhang, Xiaojuan Zhu, Pengfei Zhang, Gang Liu, Fuyou Zhou, Xiang Yuan, Ruinuo Jia, Jan Potempa, David A. Scott, Richard J. Lamont, Huizhi Wang, Xiaoshan Feng. Presence of Porphyromonas gingivalis in esophagus and its association with the clinicopathological characteristics and survival in patients with esophageal cancer. Infectious Agents and Cancer, 2016; 11 DOI: 1186/s13027-016-0049-x. 2. Significance of early healing events on periodontal repair: a review. J Periodontol 1992;63:158–65. Terranova VP. Biologically active factors in the treatment of periodontal disease. Curr Opin Periodontol 1993:129–35. Terranova VP, Wikesjo UM. Extracellular matrices and polypeptide growth factors as mediators of functions of cells of the periodontium. A review. J Periodontol 1987;58:371–80. Murakami S, Takayama S, Ikezawa K, Shimabukuro Y, Kitamura M, Nozaki T, et al. Regeneration of periodontal tissues by basic fibroblast growth factor. J Periodontal Res 1999;34:425–30. Takayama S, Murakami S, Miki Y, Ikezawa K, Tasaka S, Terashima A, et al. Effects of basic fibroblast growth factor on human periodontal ligament cells. J Periodontal Res 1997;32:667–75. Oates TW, Rouse CA, Cochran DL. Mitogenic effects of growth factors on human periodontal ligament cells in vitro. J Periodontol 1993;64:142–8. Takayama S, Murakami S, Nozaki T, Ikezawa K, Miki Y, Asano T, et al. Expression of receptors for basic fibroblast growth factor on human periodontal ligament cells. J Periodontal Res 1998;33:315–22. Shimazu A, Morishita M. Basic fibroblast growth factor induces the expression of matrix metalloproteinase-3 in human periodontal ligament cells through the MEK2 mitogen-activated protein kinase pathway. J Periodontal Res 2003;38:122–9.
- The impact of chewing gum on halitosis parameters: a systematic review
Francisco Wilker Mustafa Gomes Muniz1, Stephanie Anagnostopoulos Friedrich, Carina Folgearini Silveira and Cassiano Kuchenbecker Rösing
Published 22 February 2017 • © 2017 IOP Publishing Ltd.
Journal of Breath Research, Volume 11, Number 1.
- National Institute of Dental and Craniofacial Research – Burning mouth syndrome. NIH Publication No. 16-6288. July 2016.
- Chow AW. Infections of the oral cavity, neck, and head. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. Philadelphia, PA: Elsevier Saunders; 2015:chap 65.
Chou R, Cantor A, Zakher B, Mitchell JP, Pappas M. Preventing dental caries in children <5 years: systematic review updating USPSTF recommendation. Pediatrics. 2013:132(2);332-350. PMID: 23858419 www.ncbi.nlm.nih.gov/pubmed/23858419.
Tinanoff N. Dental caries. In: Kliegman RM, Stanton BF, St Geme JW, Schor NF, eds. Nelson Textbook of Pediatrics. 20th ed. Philadelphia, PA: Elsevier; 2016:chap 312.
- Scientific Reports 7, Article number: 41955 (2017) doi.10.1038/srep41955. In vivo remineralization of dentin using an agarose hydrogel biometic mineralization ineralization system. Min Han, Quan-Li Li, Ying Cao, Hui Fang, Rong Xia and Zhi-Hong Zhang.
- It is reported that one hundred and fourteen million Americans don’t have insurance coverage for their teeth! Sam Hodgson for The New York Times.
Our teeth are making us sick. May 23rd 2017. Zoe Greenberg. https://kristof.blogs.nytimes.com/2017/05/23/our-teeth-are-making-us-sick/?_r=0